
THE Coledale clinic is getting straight to the point on its latest project.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
It wants to see hepatitis C wiped-out from its community.
The clinic was recently named as one of just four in Australia to lead a trial aimed increasing access to treatment in Aboriginal communities, where hepatitis C statistics are over-represented.
READ MORE:
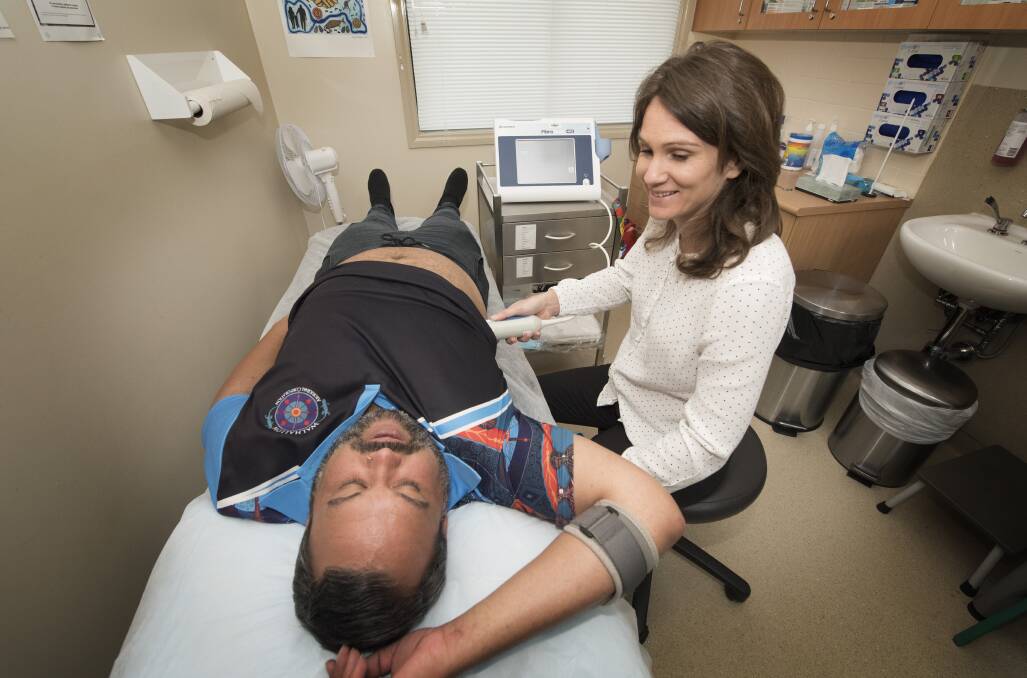
For the next three years, the clinic will be home to a "point of care" hep C testing machine, doing away with the previous rigmarole which stood between people and a diagnosis.
With a simple finger-prick blood test, a hep c diagnosis can be handed-down within an hour.
It's a time-frame which would have been unheard of in years gone by, practice manager Vanessa Wiegold said.
"They would have to see the doctor and get a blood test request and go down to pathology and then wait for the result to come back," she said.
"So quite often there were barriers there, if they didn't have any transport or they didn't follow through with their blood test, whereas now it is just a finger prick and we can have the result immediately."
The clinic has striven to eliminate any barriers for locals when it comes to the point of testing hep C trial.
It's completely free, you don't have to be on the Coledale GP's books, people just need to visit the clinic to get the test.
The treatment of the virus changed in 2016 with a highly-effective tablet-based remedy finally put on the PBS after years of lobbying.
The eight-to-twelve week antiviral sofosbuvir prescription is claimed to have cured hep C in 95 per cent of cases.
While hep C mightn't be the death sentence it once was, it remains disproportionately prevalent in Aboriginal populations.
About 10 per cent of people living with hep C in Australia are Aboriginal despite making-up 2-3 per cent of the total population.
Researcher and infectious disease physician Marianne Martinello said about 20 per cent of people living with hep C in Australia were un-diagnosed.
The nation's rate of diagnosis is relatively high, but the project, Scale C, will hopefully screen at-risk groups which could make-up that potentially treatable population.
"There still are 20 per cent of people who may not know they have been infected," Dr Martinello said.
"They may have no signs or symptoms at all ... some people may only feel very vague symptoms like fatigue, low energy and brain-fog.
"It's not until people often develop cirrhosis or liver failure that they do develop specific signs and symptoms like abdominal swelling or jaundice."
The project led by Associate Professor James Ward at the South Australian Health and Medical Research Institute.
Assoc. Prof Ward is an expert in Aboriginal health and sexually transmissible infections and blood borne viruses.


